 
The CSF hypocretin is usually unnecessary and can be used to confirm the diagnosis of narcolepsy but not IH. Usually, the MSLT should have five daytime nap opportunities in IH, and the mean sleep latency is less than 8 minutes with SOREMPs or less than two.Īctigraphy can be helpful as multiple-day recordings occur in a home environment and can corroborate the history with sleep logs- at least over seven days with unrestricted sleep. 
Valid MSLT requires that it is performed on the day following nocturnal PSG (with sufficient sleep >6 hours). Other common findings on PSG include a short sleep latency, increased total sleep time (TST), spindles, and increased sleep efficiency. In addition, PSG can help in ruling out sleep-disordered breathing (SDB) and the presence of SOREMs in narcolepsy. However, MSLT is not a sensitive diagnostic test for IH. Therefore, objective tests such as polysomnography (PSG) followed by multiple sleep latency tests (MSLT ) are very important to measure the mean sleep latency and the number of sleep onset REM periods (SOREMs) in addition to the use of a wrist actigraphy in association with a sleep log are essential to distinguish IH from other disorders that cause similar symptoms including depression, insufficient sleep, sedating medication, and sleep-related breathing disorders.Ī total sleep time must be longer than or equal to 66O minutes, especially when the mean sleep latency on the MSLT is longer than 8 min. The diagnosis of IH is by excluding other reasons and causes of hypersomnia. However, history alone is insufficient to make the diagnosis of idiopathic hypersomnia. On polysomnography, they are more likely to have increased slow-wave sleep and present with a longer sleep latency on the multiple sleep latency test. Other symptoms such as automatic behaviors, sleep paralysis, and hypnogogic hallucinations- are common but non-specific.Ĭompared to narcolepsy, individuals with IH were more likely to have prolonged and unrefreshing daytime naps and have a family history of sleepiness. Specifically, individuals with IHwLST can present with a history of severe sleep inertia, fatigue, and evening chronotype tendency. Furthermore, a study of five-hundred sixty-three participants with idiopathic hypersomnia, brain fog, and sleep drunkenness were more common in IH associated with long sleep durations. Īlthough sleepiness is the hallmark of IH, symptoms of this condition are not limited to excessive daytime sleepiness and are frequently persistent despite treatment. Īge at disease onset is usually reported to be younger in the IHwLST group, and MSLT latency is longer, with naps that are non-refreshing. 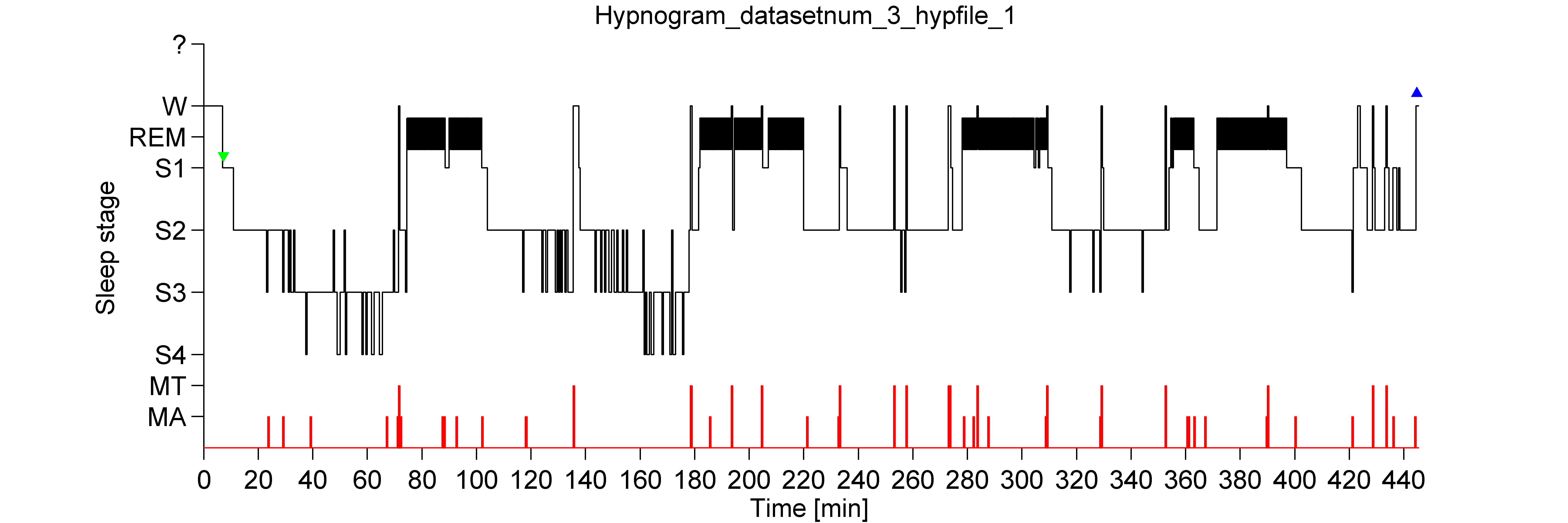
Individuals with long sleep time (>10 to 11 hours) tend to be younger at the time of disease onset, thinner, and have higher sleep efficiency. Two clinical subtypes of IH have been previously reported as IH with long sleep time (IHwLST, >10 hours) and IH without long sleep time (IHwoLST) in the second edition of ICSD. Patients commonly endorse symptoms of long daytime naps (>1 hour) which are typically non-refreshing but sleep attacks are not frequently reported. The onset of the disease is insidious, with symptoms appearing over weeks to months, making it difficult to elucidate any specific triggering factors. The usual presentation is chronic and disabling excessive daytime sleepiness in an adolescent or young adult, with the majority complaining of "sleep drunkenness" as difficulty waking up from sleep with transient confusion upon awakening. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
